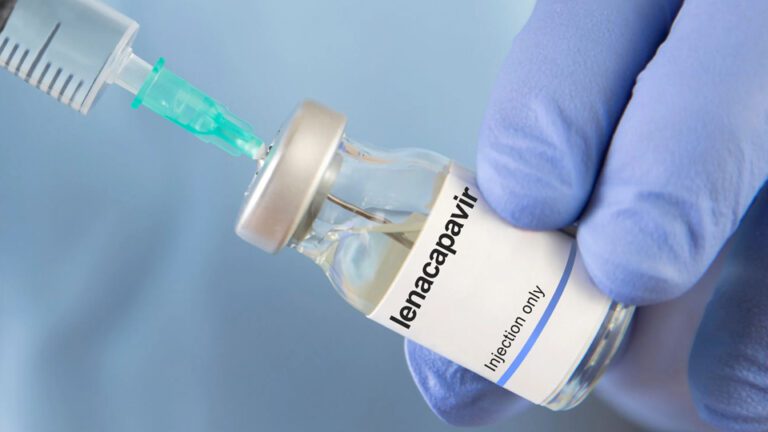
The HIV prevention and treatment drug, lenacapavir, is generating optimism among health experts and young advocates in Zimbabwe, but concerns are mounting over limited access that could undermine its potential impact.
Lenacapavir, a long-acting injectable, is being hailed as a major shift in HIV care, offering an alternative to daily oral medication.
Its introduction follows strong calls from young people across Africa, who in the Lusaka Declaration emphasised the urgent need for more convenient and stigma-free treatment options.
“Young people have been very clear about the challenges they face with daily pills, including stigma and treatment fatigue. Long-acting options like lenacapavir are not just innovative, they are necessary,” said Phakamani Moyo, an HIV advocate.
Zimbabwe is among several African countries that have begun rolling out lenacapavir, marking a significant milestone in the fight against HIV. However, access remains highly restricted. In Bulawayo, the drug is currently available at only two health facilities, raising concerns about equity and reach.
Another youth HIV advocate, Tinashe Dube, warned that limited availability could widen existing gaps in HIV prevention and treatment.
“Innovations like lenacapavir give hope, especially to young people who struggle with adherence. But if it is only available in a few centres, then it becomes a privilege rather than a solution,” Dube said.
Health advocates argue that without decentralising access to include primary health care facilities and rural clinics, the benefits of the drug may not reach communities that need it most.
This comes at a time when areas such as Bindura have been identified as HIV hotspots, underscoring the urgency of expanding prevention and treatment options.
The Lusaka Declaration highlighted that long-acting treatments could significantly improve adherence and health outcomes. However, experts warn that innovation without accessibility risks limiting real-world impact.
Advocates are now calling on the Ministry of Health and Child Care Zimbabwe and the National AIDS Council of Zimbabwe to accelerate efforts to decentralise and integrate lenacapavir into all levels of the health system.
“Lenacapavir has the potential to change the trajectory of HIV prevention in Zimbabwe,” added Moyo. “But that will only happen if access is expanded beyond a few facilities to reach every community.”